Exercise should be an essential part of the daily routine during pregnancy unless there is any medical reason not to do so. Exercise during pregnancy improves general health, vitality, and wellbeing, and reduces stress. This also prevents certain pregnancy complications. This article discusses the benefits and safety of physical activity during pregnancy.
Is a sedentary lifestyle better in pregnancy rather than staying active?
Historically women were discouraged to exercise during pregnancy. They were encouraged to maintain a sedentary habit.
Many people (including some healthcare professionals) feared over the years that physical activity could be harmful during pregnancy.
There is no scientific evidence to show that a sedentary lifestyle during pregnancy is beneficial (unless there are some pregnancy complications where reduced physical activity is advised).
In fact, sedentary habits could predispose to as excessive weight gain and pregnancy complications, such as deep vein thrombosis. Excess weight gain, in turn, could increase the risk of gestational diabetes and preeclampsia.
Therefore, all the renowned professional bodies (from all across the world) recommends pregnant women (without certain medical complications) to stay active and undertake physical exercises during pregnancy (even if they were not active physically before pregnancy).
Can you exercise while you are pregnant?
Yes, you certainly can. Scientists have proven that exercise during pregnancy is safe if suitable activity and intensity are chosen. There is no scientific evidence to suggest that moderate exercises can be harmful to the pregnant woman and her baby.
Moderate exercise during pregnancy does not increase the risk of miscarriage, preterm birth (early delivery) or low birth weight babies (intra-uterine growth restrictions).
Pregnancy is a wonderful opportunity and motivation to adopt a healthy lifestyle. Therefore, you certainly can start doing regular exercise if you have not done so in the past (unless there are certain medical conditions).
What are the conditions where exercises during pregnancy should be avoided?
Women with the following medical conditions should not perform exercises during pregnancy (ACOG Guideline):
1) Some heart and lungs diseases/ conditions.
2) If she has a cervical cerclage or at risk of miscarriage due to cervical incompetence.
3) Low-lying placenta (Placenta Previa), especially after 26 weeks of pregnancy.
4) Premature rupture of membranes (leaking of amniotic fluid) or risk/ symptoms of pre-term labour.
5) Severe anaemia.
6) Raised blood pressure/ Preeclampsia.
7) Women with Twin/ triplets pregnancies (or higher order multiple pregnancies) with the risk of pre-term labour.
Also, pregnant women with fever should avoid exercise due to the risk of fetal hyperthermia.
Women with the following conditions should reduce physical activity, avoid strenuous exercise and heavy-weight lifting:
1. Evidence of fetal growth restrictions or at high risk of developing fetal growth restrictions.
2. Women at high risk of miscarriage.
3. Women at high risk of preterm labour.
What are the benefits of exercise during pregnancy?
There are several benefits of moderate- intensity exercise during pregnancy:
1) Reducing Gestational Diabetes:
Exercise helps in both preventing gestational diabetes. This also improves blood sugar control in women with gestational diabetes.
2) Reducing Preeclampsia:
Exercise reduces the risk of developing preeclampsia and gestational hypertension.
3) Improving the Cardiorespiratory fitness (CRF):
Cardiorespiratory Fitness (CRF) is the body’s ability to supply oxygen to muscles during prolonged physical activity. The body does through effective functions of the heart (cardiac) and lungs (respiratory).
VO2 Max is the measurement of CRF of the individual. VO2 Max refers to the highest amount of oxygen a person can consume during physical exercise.
Exercise during pregnancy improves CRF which helps in the better adaptation of the body to the normal physiological changes and in labour.
Exercise also improves other bodily functions, such as muscular strength and endurance, flexibility, agility, coordination, balance, reaction time, and speed.
4) Prevents excessive weight gain during pregnancy:
Excess weight gain during pregnancy increases the risk of gestational diabetes, preeclampsia, and other medical complications. Exercise and adherence to a healthy diet prevent the excessive weight gain.
5) Improves wellbeing:
Exercise during pregnancy improves mood, psychological wellbeing and depression symptoms. Mind-body interventions, such as yoga, are known to reduce stress.
6) Reduces urinary incontinence:
Pelvic Floor exercises, performed regularly, prevents/ improves urinary incontinences both during pregnancy and after the childbirth.
7) Improvement in sleep:
Exercise is thought to help with sleep and prevents insomnia. However, strenuous exercise in the evening could lead to sleep disturbance/ insomnia at night, so should be avoided.
8) Reduces back-pain
There is some evidence to suggest that exercise during pregnancy could help in back pain.
9) Helps to reduce weight (gained during pregnancy) after the childbirth.
10) May reduce the risk of a Caesarean birth.
Considering the above benefits, it is advisable to exercise during pregnancy and stay physically active, unless there are medical reasons not to do so.
What kinds of exercises are safe during pregnancy? What type of physical activity is recommended during pregnancy?
Scientific bodies from all across the world suggest the following during pregnancy:
1) Breaking the sedentary lifestyle
It is advisable that every reasonable opportunity should be taken to be active throughout the day.
Prolonged sitting should be avoided. It is important to remember that every physical activity counts. Light physical activities (such as light household chores and cooking) does not count towards the recommended exercise routine during pregnancy. But they are key to staying active and break the cycle of the sedentary lifestyle.
2) Aerobic exercise:
During pregnancy, 150 minutes (per week) of moderate-intensity aerobic exercise is recommended (this should be spread throughout the week). This can be performed in as little as ten-minute bouts. (Ref)
3) Muscle strengthening exercise/ activity
Pregnant women are recommended to carry out 8 – 12 repetitions of these activities. They should involve all major muscle groups in the body. This should be done at least twice per week. (Ref)
In practical terms, a typical exercise session during pregnancy consists of the following:
– Beginning with a warm-up, muscle-strengthening exercise/ stretching for 5 – 10 minutes.
– Then performing aerobic exercise for about 30 minutes
– This is followed by rest and cooling down period for about 5 – 10 minutes.
What is aerobic exercise?
The word ‘Aerobic’ means ‘involving oxygen’. Aerobic exercise (also called ‘cardio’) refers to physical activities taken to improve the efficiency of the body in utilising oxygen in the formation of energy.
Aerobic exercises usually involve moving large muscles of the body (such as legs and arms) at a moderate intensity to increase the heart and breathing rates.
These exercises ensure that the body utilises a process called aerobic metabolism. Aerobic exercises involve oxygen supply to break down glucose to produce the basic energy molecules of the cells called ATP (Adenosine Triphosphate).
ATP: the body’s energy currency
During exercise or any physical activity, the muscles require energy.
The energy of the muscle cells comes from a molecule called ATP (Adenosine Triphosphate). ATP has a short half-life, therefore cannot be stored within the muscle cells for long. Therefore, ATP needs to be produced constantly (within the muscle cells) from glucose during the entire exercise session.
ATP is produced from glucose in two pathways:
– Aerobic metabolism
– Anaerobic metabolism
Aerobic metabolism requires oxygen. Anaerobic metabolism can produce ATP without oxygen.
Aerobic is the most efficient form of metabolism, compared to the anaerobic variety.
For example, 1 molecule of glucose produces 38 molecules of ATP in aerobic metabolism.
On the other hand, during anaerobic metabolism, only 2 molecules of ATP are produced.
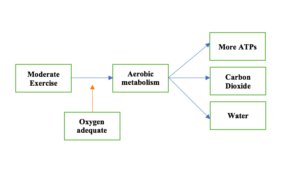
During exercise, the breathing rate increases. This ensures a high amount of oxygen available to the muscle cells. If the oxygen level is adequate, the aerobic metabolism is activated. During this process, a high amount of ATP is produced, along with water and carbon dioxide.
The by-products of the aerobic metabolism (i.e., carbon dioxide and water) are easier to excrete from the body. For example, carbon dioxide is easily excreted through the lungs during the high breathing rate at the time of exercise. This excretion does not require any further oxygen.
However, when the exercise continues (or intensity is increased), the tissue oxygen level is no longer remains enough for the aerobic metabolism (in spite of the high breathing rate).
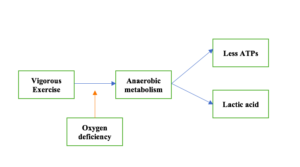
In this circumstances, to ensure a continuous supply of ATPs, the anaerobic metabolism is activated within the muscle cells.
During the anaerobic metabolism, less ATP is produced (compared to the aerobic metabolism). Also, the by-product of the anaerobic process is lactic acid. The lactic acid causes pain, soreness, and fatigue in the muscles.
Moreover, the lactic acid is only broken down and excreted from the body with the help of oxygen.
Therefore, the body needs to stop the exercise and take some rest to replenish the oxygen level. Therefore, after a strenuous workout, we need to take rest to recover.
It is important to remember:
During the pregnancy, the energy demand of the tissues is more in the same type and intensity of the aerobic exercise. This is due to increase in body weight, blood volume, requirements of the placenta and the growing baby. Therefore, non-weight-bearing exercises are better performed during pregnancy compared to the weight-bearing ones.
With the practice of regular aerobic exercise, the Cardiorespiratory Fitness (CRF) of the body improves. Then the muscles can utilise oxygen better and can delay the anaerobic process longer with higher intensity exercises.
Which aerobic exercises are safe during pregnancy? Which exercises are best for a pregnant woman?
Moderate intensity low-impact aerobic exercises that are safe during pregnancy are:
– Brisk walking
– Swimming and aqua-natal exercises
– Workout on stationary exercise bikes
– General gardening activities (such as weeding, raking or digging)
The low impact exercise refers to all the physical activities where at least one foot is always in touch with the ground. During the low impact exercises, there is a reduced risk of fall and injury to the pregnant woman.
I was never been active before pregnancy. Can I start doing exercises during pregnancy?
Yes, of course, you can make a start unless you have certain medical conditions (mentioned above). However, if you are starting exercises for the first time, you are advised to start gradually. This would allow your body to get used to the changes to build better exercise tolerance.
You should, however, not start performing vigorous/ high-intensity exercise and heavy-weight training during pregnancy, if you have not done them before pregnancy.
I would like to start to exercise. Which month to start exercise during pregnancy?
This is brilliant that you have decided to start doing exercise during your pregnancy. You can make a start at any stage of pregnancy (i.e., first, second or third trimester). However, you should get medical advice before starting physical exercise if you have any of the following:
– High BMI
– Any medical condition
– Risk of miscarriage or preterm labour
– Cervical cerclage
Is it safe to perform vigorous/ high-intensity exercises during pregnancy? Can you still go to the gym while pregnant?
It is generally agreed that the pregnant women who have been doing high-intensity exercises before the pregnancy may continue them during pregnancy with some adaptations (so long they do not have/ develop any medical complication). However, there is very limited scientific evidence available on the impacts of intense physical activity during pregnancy.
If you are already doing high intensity/ high impact exercises before pregnancy (and would like to continue), please speak with your Obstetrician, midwife, the health care provider, your Trainer or a sports medicine specialist at the earliest.
It is advisable that you consider modifying high-intensity workouts as the pregnancy advances.
Moreover, vigorous workouts often involve high impact exercises (i.e., during these exercises, both feet are off the ground at the same time). The examples of the high impact exercises include jogging, sprinting, aerobic dancing (such as Zumba), jumping, skipping etc.
There is a high risk of fall and an accidental trauma to the abdomen (during the high impact exercises).
Vigorous/ high impact exercises should be avoided for the beginners during pregnancy.
Is it ok to jog in early pregnancy?
Jogging is a high impact and high-intensity exercise. If you have been jogging for sometimes before pregnancy, you may wish to continue. This is usually considered safe unless you have certain medical conditions (where reduced physical activity is advisable). However, as with other high impact exercises, the research data is limited. Therefore, it is advisable to speak with your Obstetrician, midwife, the health care provider, your Trainer or a sports medicine specialist at the earliest.
Can you get a miscarriage from running? Can running while pregnant hurt the baby?
Running/ jogging are high-impact and high-intensity exercises. They are usually considered safe during pregnancy if you are already doing them prior to the pregnancy.
The safety data on the practice of high-intensity exercise during pregnancy is limited.
Therefore, it is advisable to avoid running/ jogging or similar high-impact and high-intensity exercises during pregnancy if you have risk factors for miscarriage or preterm labour.
They are not recommended to be started during pregnancy if you have not done them before pregnancy.
Can I still do Zumba while pregnant?
Zumba is a high-impact and high-intensity exercise. Therefore, all the advice similar to running/ jogging (as above) apply to the Zumba too.
Is it safe to do squats while pregnant?
This is a commonly advised exercise for the mothers-to-be. It is safe to perform squats unless there are certain medical conditions (mentioned above where reduced physical activity is advised). However, it could be challenging as the pregnancy advances or if you have pelvic girdle pain/ backache. Therefore, please ensure that you are comfortable during squats.
Can you do sit-ups in early pregnancy?
If you have been doing sit-ups before pregnancy, you may wish to continue in the first trimester. However, exercises in the supine (lying flat) is not advisable after the first trimester (especially after 16 weeks of pregnancy). Therefore, it would be better to discontinue after the first trimester. If you wish to carry on, then speak to your healthcare providers.
Is it safe to perform exercises during pregnancy in the water?
Aquatic exercises are a non-weight-bearing form of aerobic exercises. They are very safe and effective during pregnancy and have certain advantages:
– Little concern with the loss of balance and fall.
– Less concern for hyperthermia, as the heat can dissipate easily.
– Less impact and risk of injury to the weight-bearing joints.
What are muscle strengthening exercises?
These exercises involve moving the muscles against a resistance. The resistance can be one’s own weight, machines or weight tools.
Muscle strengthening exercises are not aerobic exercises. So they should be done in addition to the aerobic exercises during pregnancy.
‘Repetitions’ and ‘Sets’ are the two terms used to count the muscle strengthening exercises. The ‘Repetition’ refers to one complete movement of an activity, whereas a ‘Set’ is a group of those ‘Repetitions’.
Yoga, Pilates, and weight training are examples of muscle strengthening exercises.
Pregnancy yoga and pregnancy pilates are safe forms of exercises during pregnancy (when undertaken under the supervision of a trained and qualified instructor).
Difficult yoga/ pilates postures/ positions are to be avoided to avoid loss of balance and injury to the belly.
Exercises in the supine position (lying flat on the floor) are also not advisable to avoid the postural drop of blood pressure (postural hypotension). This reduces blood flow to the brain (can result in fainting episode) and uterus/ placenta (can result in fetal compromise).
However, caution needs to be taken for the weight training during exercise.
Is it safe to perform weight training during pregnancy?
Weight training may be performed during pregnancy. However, there is very limited information on its’ safety. Therefore, an individualised approach is necessary for every single pregnant woman who is keen to perform the weight training.
It would be advisable to discuss such workouts with health care providers, training instructors and/ or a sports medicine specialist.
In absence of good scientific evidence on safety, it might be useful to consider alternative muscle strengthening exercises during pregnancy.
In general, if the weight training is attempted during pregnancy, then the following should be advised:
– use low weights (machine or free equipment)
– use multiple repetitions
– apply a different range of movements
– take short breaks and avoid long workouts.
Extreme caution is required for heavy weight lifting exercises during pregnancy. Sudden stoppage of deep breathing (‘Valsalva maneuver’) during these sessions, could increase blood pressure and reduce blood flow to the fetus.
What is the safe upper limit of exercise intensity?
There is no safe upper limit for the exercise intensity during pregnancy has been established. This is due to the fact that the exercise endurance is different for every individual.
While the same intensity of exercise could be perceived as mild-to-moderate by a trained individual, it could be of high intensity for another person who does not perform regular exercise.
The heart rate normally increases during pregnancy (even at rest) due to physiological changes. Therefore, this is not a very good predictor of exercise intensity during pregnancy.
Talk Test
A simple method of assessing the exercise intensity during pregnancy is ‘Talk Test’. A pregnant woman should be able to maintain a normal conversation during her entire moderate-intensity aerobic exercise session. If she is out of breath and cannot talk properly, then the exercise is likely to be performing a high-intensity workout.
Borg Rating of Perceived Exertion Scale
It is your personal perception of the intensity of a physical activity. Borg Rating of Perceived Exertion Scale is a very practical method to assess the workout intensity. For moderate-intensity exercises during pregnancy a Borg rating of 13-14 is desirable. The rating of 20 indicates maximal intensity, whereas 6 indicates no exertion.
Why performing exercises during pregnancy could be challenging?
Due to physiological changes in the body during pregnancy, sometimes exercising could be challenging. The following are the reasons:
A) More breathlessness symptoms during pregnancy: (Ref 1)
About 70% of healthy pregnant women suffer from the symptoms of breathlessness (‘Dyspnoea’), even when they are resting. This happens without any respiratory illness or other health disorder.
Women can get breathless very easily during pregnancy at the time of exercise.
Mechanism:
These symptoms are primarily due to an increase in the minute volume, which is the total volume of air inhaled or exhaled during breathing every minute. The minute volume is increased by about 30% at rest during pregnancy.
This is mainly due to the increase in the Tidal Volume (TV), which is the amount of air inhaled or exhaled during each breath (TV increases by 45% during pregnancy).
In simple terms, Minute Volume = TV x Rate of breathing per minute (‘Respiratory Rate’).
The respiratory rate during a healthy pregnancy remains almost unchanged.
This increase in the minute volume is needed to serve the following purposes:
1) To increase oxygen supply in the body:
During pregnancy, the oxygen requirement of the body increases by 30% to 40%. This gradually rises as the pregnancy advances. This is required to meet the demands of the increased metabolic function of the body (‘Basal Metabolic Rate’).
The basic metabolic rate during pregnancy increases due to:
a) the needs of the growing fetus, uterus, and placenta.
b) increased function of the heart, lungs and other systems during pregnancy.
2) To wash out the excess carbon dioxide production:
During pregnancy, the body’s carbon dioxide production increases by about 30-300 ml/minute. This happens due to increased Basal Metabolic Rate of the body. The increased minute volume helps to wash out this excess carbon dioxide gas from the body.
B) More prone to fall
A pregnant woman has more tendency to fall compared to the non-pregnant state. The disturbance in the body balance occurs due to the following:
– There is a shift in the body’s centre of gravity due to the growing fetus.
– The laxity of the joint increases due to hormonal changes.
In fact, the injury due to fall is 2-3 times more likely in pregnant women compared to their non-pregnant counterparts.
C) Pregnancy ailments
Due to the common pregnancy symptoms (such as nausea/ vomiting and backache), exercise could be challenging. Sometimes she also could suffer from insomnia. As a result, she could be exhausted and tired.
She might also develop swelling of the feet (oedema) or could suffer from stiffness/ pain in the wrists (‘Carpal tunnel syndrome’) during pregnancy. They could make joint movement and the exercise difficult.
D) Cardiac changes
The blood volume increases by 50% more than the non-pregnant state. Therefore, the heart needs to work harder to deal with this overload. The heart does so by increasing the heart rate and the amount of blood pumped out of the heart every minute (‘cardiac output’). The heart rate increases by 10-20 beats per minute and the cardiac output increases by 30-50%. (Ref 2)
Resting heart rates and heart rates at lower exercise intensities are higher during pregnancy, which reduces the available margin of increase during exercise. Heart rate recovery after exercise increases as pregnancy progresses, while physical recovery time indicates no change. (Ref 3)
What are some basic tips for exercises during pregnancy?
1. Drink plenty of water before, during and after exercise sessions. This would prevent dehydration.
2. Wear supportive clothing during the exercise session. For example, use a sports bra for supporting breasts and belly support belts for reducing abdominal discomfort (especially in the third trimester).
3. Adopt measures to allow better dissipation of heat. For example, during the exercise wear loose-fitting clothes, avoid exercising in a hot/humid environment, perform exercising in water and/ or exercise in a temperature-controlled room (if the external temperature is high).
4. Listening to the body: to stop when you feel exhausted/ tired.
What are the risks/ concerns for exercises during pregnancy?
Risks of exercise during pregnancy include the following:
A) Trauma:
Pregnant women can sustain trauma from contact sports and/or due to the tendency to fall/ postural hypotension.
B) Raising core body temperature: (Ref)
During pregnancy, there is an improvement of the body’s mechanism to dissipate heat (Thermoregulatory system). This happens due to the following:
1) Increased blood flow to the skin surface.
2) Increase in the exhaled air volume during breathing (‘Minute ventilation’)
3) Lowering of the set point for the normal temperature of the body.
4) Increased blood volume
The internal body temperature (‘Core temperature’) usually increases by 1.5° C during the first 30 minutes of moderate-intensity exercise in normal external temperature. If the exercise is continued further, then, the core temperature does not increase anymore and reaches a plateau. This is due to the effective system of heat dissipation. (Ref 4)
The fetal temperature is on an average 1° C higher than the mother’s core temperature.
Therefore, moderate-intensity exercise regime (in normal external temperature) does not increase fetal temperature significantly.
When the exercise is undertaken in a hot and humid condition or during high-intensity exercise, the heat dissipation system does not work effectively.
This can get worse in presence of maternal dehydration. Dehydration interferes with heat dissipation even further resulting in a further increase in core temperature.
As a result, the pregnant woman’s core temperature continues to rise. Consequently, the fetal temperature keeps on increasing.
There are some studies to suggest that maternal core temperature (during the first 45-60 days of pregnancy) over 39° C (100° F) can lead to fetal malformations. (Ref 5)
All such studies investigated the impact of fever during early pregnancy. There is no evidence to suggest that transient raised temperature due to exercise during pregnancy is harmful to the fetus.
It is usually recommended that pregnant women should avoid exercise at an external temperature exceeding 90°F (32°C). The hydrotherapy pool temperatures should be kept ≤95°F (35°C) if this is used by a pregnant woman.
C) Blood flow to the uterus and placenta
During exercise, the blood flow shifts to the muscles. As a result, there could be a reduced blood supply to the uterus and placenta at the time of exercise during pregnancy.
However, the studies have shown that the fetus compensates well to this transient reduction in utero-placental blood flow. There is no evidence to suggest that moderate-intensity exercise during pregnancy predisposes fetus to any risk of hypoxia (lack of oxygen) or causes fetal distress.
This is a reason why prolonged strenuous exercise should be avoided in pregnancy.
What precautions are to be taken for exercises during exercises?
Things to be avoided in exercises during pregnancy:
A) Avoid exercise in the supine (lying flat) position:
In the supine position, the enlarged uterus puts pressure on the inferior vena cava (major blood vessel in front of the spine). As a result, the return of blood from lower limbs (‘Venous return’) to the heart is decreased.
Due to this, the blood pressure could drop (‘orthostatic hypotension’) and the blood flow to the fetus could be reduced.
B) Avoid contact sports:
This could increase the risk of injury to the abdomen. Therefore contact sports, such as soccer, karate, boxing, tennis etc. should better be avoided.
C) Avoid sports with high risk of fall:
As the body balance could be disturbed and tendency to fall increases during pregnancy, sports activities with high risk of fall should be avoided. These include gymnastics, skiing, off-road cycling, surfing, and horse riding.
Professional pregnant sportswomen involved in those activities should get advice from experienced trainers/ sports medicine specialists.
D) Avoid factors which can lead to hyperthermia:
1. Avoid exercise in a hot humid environment:
Risk of increased temperature (‘hyperthermia’) which could, in turn, raise the fetal temperature. There is some concern that this could harm the fetus, especially in the first trimester. However, more research is needed in this area.
2. Avoid dehydration during exercise:
This could worsen the adverse effects of maternal hyperthermia.
3. Avoid ‘Hot Yoga’ and ‘Hot Pilates’.
E) Avoid scuba diving and skydiving:
This could result in the formation of the air bubbles in the blood. Babies do not have mechanisms to filter those air bubbles. This could affect the baby by occluding the blood flow to the organs, especially to the lungs (Air embolism).
F) High altitude:
To avoid exercises on the initial 3-4 days of arrival to a high altitude (above 6000 feet). This would allow adaptation to the low atmospheric pressure and reduce the risk of acute mountain sickness. This is an emergency medical condition.
G) High impact exercises:
They could increase the risk of injury to the joints and chance of fall. Therefore, they should better be avoided, especially for the beginners during pregnancy.
When to stop during an exercise session during pregnancy?
In the following circumstances, exercise should be stopped and urgent medical attention would be required:
– Active vaginal bleeding
– Symptoms of leaking amniotic fluid from the vagina
– A headache
– Lightheadedness/ dizzy spells
– Breathing difficulty during or before exercise
– Regular painful contractions
– Chest pain
– Swelling/ pain in calf muscles.
– Feeling very tired/ exhausted.
What advice should be given to the elite athletes?
Pregnant athletes or those involved in competitive sports should get adequate advice from their health care providers, trainers, and sports medicine specialist. This would help them to develop an individualised safe training regime.
They should be given information on the impact of high-intensity exercise during pregnancy.
It is usually advised not to aim for the maximum pre-pregnancy fitness levels.
Is exercise in water beneficial during pregnancy?
Summary and conclusion
1. Pregnant women should be advised to stay active and perform a regular moderate-intensity exercise during pregnancy (unless they have any medical complication where exercise should be avoided).
2. Exercise during pregnancy have several health benefits. This could reduce gestational diabetes and preeclampsia and improves mood, wellbeing, and sleep.
3. Moderate-intensity aerobic exercise during pregnancy do not cause miscarriage, preterm birth/ delivery or fetal growth restriction (‘Small for dates’ baby).
4. There is limited scientific data on the safety of high-intensity exercise and heavy-weight training during pregnancy. They should be avoided for the beginners.
For trained professionals, these activities may be continued with some modifications. However, it is always advisable to seek advice from healthcare providers/ Trainers/ Sports Medicine specialists.
5. Physical activities to be avoided during the pregnancy are contact sports, high impact exercises, Scuba and Sky Diving, ‘Hot Yoga’ and ‘Hot Pilates’.
6. Heart rate measurement is not a good indicator of exercise intensity during pregnancy (as maternal heart rate increases during pregnancy). Perception of intensity and Talk Test are simple and practical ways to assess the intensity.
7. Exercise could lead to a rise in maternal body core temperature (‘Hyperthermia). Hyperthermia (especially from fever due to illness) is thought to be harmful to the fetus, especially in the early pregnancy.
However, exercise-induced transient hyperthermia is not known to be harmful. Still, it is advisable to take measures to dissipate heat effectively during exercise during pregnancy.
8. For pregnant women with no medical complication and no contraindications for exercise, the recommended activities should include a combination of both aerobic exercises (total of 150 minutes per week) and muscle strengthening exercises (8-12 repetitions at least twice per week).
9. There is no established safe upper limit of exercise intensity during pregnancy. Pregnant women are advised to listen to their bodies and avoid over-exerting themselves.
10. Performing exercises should be stopped if there are any medical/ pregnancy complications, such as chest pain or vaginal bleeding, leaking amniotic fluid or signs of labour.
11. There are some medical conditions where exercise during pregnancy should be avoided, such as fever, active vaginal bleeding, placenta previa, ruptured amniotic membrane, fetal growth restriction, high risk of miscarriage (such as cervical incompetence), high risk of preterm labour and high blood pressure.
References
1. G. Bourjeily, K. Rosene-Montella (eds.), Pulmonary Problems in Pregnancy, Respiratory Medicine, DOI 10.1007/978-1-59745-445-2_2 Humana Press, a part of Springer ScienceþBusiness Media, LLC 2009
2. Robson SC, Dunlop W, Boys RJ, Hunter S. Cardiac output during labour. Br Med J (Clin Res Ed) 1987;295:1169–72.
3. Bonds, D., & Delivoria-Papadoupoulos, M. (1985). Exercise during pregnancy. Potential fetal and placental metabolic effects. Annals of Clinical and Laboratory Science, 15(2), 91-99.
4. Soultanakis, H.N., Artal, R., & Wiswell, R.A. (1996). Prolonged exercise in pregnancy: Glucose homeostasis, ventilatory and cardiovascular responses. Seminars in Perinatology, 20, 315–327.
5. Milunsky, A. et al. (1992). Maternal heat exposure and neural tube defects. Journal of the American Medical Association, 268, 882–885.


