Addressing stress during pregnancy can prevent many complications. This article briefly outlines what is stress, stress symptoms and treatment and if the stress can harm unborn babies.

Myths and facts of stress
Before we discuss the impact of the stress during pregnancy, it would be useful to understand some basic aspects of stress.
What is stress?
The stress is the body’s ‘fight or flight’ response with regards to a threat, challenge or pressure. Any such threat, challenge or pressure, which causes a stress response is called a ‘stimulus’ or a ‘stressor’.
The stimulus/ stressor is of two types:
External (stimulus present outside the human body): such as environmental temperature or external hazard.
Internal (stimulus present inside the human body): such as fearful thoughts, pain.
The stimulus could also be a real or imaginary/ anticipatory one.
The aim of this stress (or ‘fight or flight’) response is to prepare the body to deal with the stressor effectively. This involves a number of changes in different organs of the body so that the person can either fight with or move away from the stressor.
1) Myth: Certain distressing symptoms are stress:
For many of us, the stress means overwhelming, uncomfortable and distressing mental (such as feelings of worry, tension, nervousness, inability to relax and the fear/ anticipation of potential harm, inability to think properly) and physical (such as palpitation, sweating and shaking) symptoms.
Fact: These mental and physical symptoms are the result of the stress response of the body (‘Allostasis’), rather than the stress itself.
2) Myth: Stress and anxiety are the same:
Fact: The two words, stress and anxiety, are often used interchangeably. However, in scientific terms, these two are two distinct entities:
Stress is the body’s response to a stressor.
Anxiety is a group of symptoms in absence of any stimulus/ stressor. Anxiety (often called ‘anxiety disorders’) is a mental health condition.
Chronic/ persistent stress can lead to anxiety disorders. Stress and anxiety can co-exist.
3) Myth: Stress is always bad
Fact: The stress response is a vital life-saving survival strategy when someone is faced with a danger. However, the same response is activated in anticipatory/ imaginary threats or fear or in unpleasant life experiences, too.
In other words, the stress response is activated is any situation (including real dangers) where the brain perceives that the body would be unable to cope safely.
In absence of a real danger, the symptoms resulting from a stress response become very uncomfortable.
On the other hand, chronic stress could be harmful and can lead to some health disorders.
However, the word ‘stress’ is usually used to describe (and discussed in the context of) unpleasant/ distressing symptoms and health risks.
4) Myth: Certain experience/ life events are stress
Fact: Often the stressors/ stimuli leading to the stress response are referred to as stress. It is important to remember that stress is the body’s response and not the factors (stressors) which activate this mechanism.
What are ‘Homoeostasis’ and ‘Allostasis’?
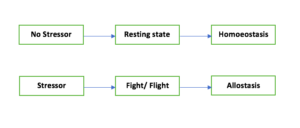
In absence of a stressor, the body maintains it’s normal functions through a process called ‘Homoeostasis’.
Therefore, the homoeostasis is defined as the body’s mechanism of maintaining the internal environment within safe limits, especially in absence of stressors.
The body’s mechanism responsible to handle a stressor is called ‘Allostasis’. This is the body’s ability to adapt to the challenges (both external and internal).
How does the body respond to a stressor/ stimulus?
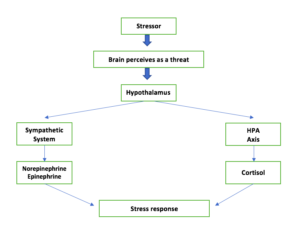
The process involved in this stress response involves the following:
1) The brain perceives the stimulus as a potential threat which can be harmful to the body.
2) The brain sends a signal to the hypothalamus (a part of the brain) to activate the ‘fight or flight’ response in the body.
3) Hypothalamus does the following:
A. Activation of the sympathetic nervous system:
This leads to the release of the hormones, norepinephrine (noradrenaline) and epinephrine (adrenaline).
These hormones cause the following changes:
– A shift of blood flow from less urgent functions/ systems (such as digestive systems) to the organs needed to function more during stress (such as muscles).
– A rise in heart rate, pumping of the blood (‘cardiac output’), the blood pressure, the rate of respiration and sweating.
B. Activation of ‘hypothalamic-pituitary-adrenal (HPA) axis’:
Hypothalamus activates this by the release of the hormone Corticotropic Releasing Hormone (CRH). CRH activates the Pituitary gland to secrete another hormone called Adrenocorticotropic Hormone (ACTH). ACTH, in turn, activates the adrenal gland to secrete the hormone Cortisol.
Cortisol ensures that there is a constant supply of energy to all the organs at the time of stress. The source of the body’s energy is glucose. Cortisol helps to break down glucose stores in the body (called ‘glycogen’) and stops glucose entry into the cells. These actions lead to raised glucose levels in the blood.
What changes happen normally during pregnancy?
Even without any stressor, the following changes occur during pregnancy:
– Sympathetic nervous system:
There is a gradual increase in the activity of the sympathetic nervous system as the pregnancy progresses. This results in increased heart rate and blood volume when the heart pumps (‘stroke volume’). However, it is not clear if this leads to an increased anxiety during pregnancy. (Ref 1)
– HPA Axis:
During pregnancy, the placenta releases Corticotropin-Releasing Hormone (CRH), in addition to the hypothalamus. This acts on the pituitary to release more ACTH. Subsequently, there is more release of cortisol. Therefore the blood level of cortisol gradually increases during the pregnancy, reaching its peak nearer the 40 weeks. (Ref 2)
What are the different types of stress?
Stress is of two types:
1) Acute Stress: One-off/ infrequent activation of the stress response
Once the stressor disappears (and the brain does not perceive any further threat/ danger), then the stress response stops.
In other words, the allostatic mechanism stops and the homoeostatic process starts. As a result, the body goes back to it’s resting state.
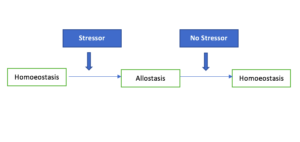
2) Chronic Stress: When there is repeated and frequent exposure to the stressors (‘Allostatic load’), the stress response is activated repeatedly.
As a result, the body cannot go back to the homoeostatic/ resting state and goes to a state of chronic stress (Allostatic overload’).
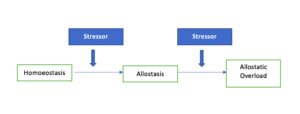
Chronic activation of the stress response (Chronic stress) could lead to severe disruption of the quality of life and certain health conditions, such as diabetes, heart disease, and mental health illnesses.
Stress during pregnancy
What is Pregnancy-specific stress?
Many researchers now believe that the Pregnancy-specific stress (also known as Pregnancy-related anxiety) is a separate and distinct clinical identity. (Ref)
This refers to stress related to fear of the parents about the health and safety of the unborn baby, the risk of birth defects/ medical complications during pregnancy/ childbirth, adequate care and the parenting of the newborn. (Ref)
Pregnancy-specific stress is thought to be more closely linked (compared to general stress/ anxiety disorders) with adverse outcomes both for the pregnancy and the baby.
Pregnancy-Related Anxiety Questionnaire-Revised (PRAQ-R) is a 10-item shortened version of the PRAQ. This has been tested with psychometric methods. Research has shown that PRAQ-R is a reliable predictor of pregnancy and child’s outcomes. (Ref)
What causes stress during pregnancy?
In the same situation, every individual responds differently. Stressors are the perception of internal/ external events happening to an individual. Therefore, the same condition could be a stressor for some but not for the others.
However, the following are some common bio-psycho-social factors causing stress during pregnancy:
Physical:
– Insomnia
– Backache/ Pelvic Girdle Pain
– Pregnancy complications
Psychological:
1) Concerns regarding:
– Pregnancy complications and delivery, analgesia, Tocophobia.
– Ability to care for the child: feeding, arranging childcare, child safety
– Parenting skills
2) Work-related stress during pregnancy:
– Impact on employment/ career
– Return to work
– Sickness absenteeism due to pregnancy ailments
– Fear of job loss
3) Financial implications: such as return to work as a part-time, increasing cost after the baby is born
4) Poor antenatal care: especially when there are poor information and lack of continuity of care.
5) Diagnosis of fetal cardiac abnormalities or Neural Tube Defects (NTD)
6) Relationship stress during pregnancy
7) Bereavement during pregnancy
8) Restriction to social life and activities during pregnancy
9) Intimate partner violence:
About 9% of pregnant women are the victim of intimate partner violence. 30% of those start during pregnancy.
(Ref 3, 4)
Social:
– The social pressure of ‘perfect mother’
– Lack of family/ social support
Bio-Psycho-Social Stressors
No pregnant woman is immune to emotional stress during pregnancy. Stress during pregnancy can happen in the first, second and third trimester.
What are the symptoms of stress during pregnancy?
Acute stress is often short-lived but chronic symptoms could have persistent symptoms:
Psychological:
– Lack of concentration
– Indecisiveness
– Unable to relax
– Constantly feeling anxious (‘on the edge’)
– Intrusive thoughts
– Lack of confidence
– Low self- esteem
– Irritable/ angry
Physical:
– Headache/ worsening migraine
– Muscular pain
– Constant tiredness
– Insomnia
Social
– Avoidance of person/ situation
– Smoking, alcohol, drugs as a coping mechanism
Stress can have an impact on the health either directly (distressing psychological/ physical symptoms and long-term health problems) or indirectly (through unhealthy habits, such as smoking/ alcohol).

Bio-Psycho-Social impacts of stress
Can stress harm unborn babies?
Fortunately, these effects are rare. Therefore no pregnant woman should unnecessarily worry if they are undergoing emotional stress during pregnancy.
Research has shown that stress during pregnancy could lead to the following: (Ref 5)
Antenatal:
– Congenital birth defects (especially severe stress during the first trimester)
– Low birth-weight babies
– Premature birth
Effects of stress during pregnancy on infant and child development:
– Newborn: changes in the neurodevelopmental functioning
– Infants and toddlers: behavioural problems, such as temperament difficulties, sleep disturbance, poor cognitive performance, increased fearfulness
– 3-16 years: increased mental health conditions (usually anxiety and depression), ADHD and symptoms of conduct disorders.
– Adults: increased risk of schizophrenia.
What are the impacts of stress on the pregnant woman?
Stress and mental health conditions during pregnancy could lead to an unhealthy lifestyle: (Ref)
1. Less exercise, unhealthy diet (such as less intake of fruits and vegetables), and more weight gain during pregnancy.
2. Smoking and substance misuse.
How much stress is too much during pregnancy?
It is not known exactly what degree of stress during pregnancy is harmful to the child in the forthcoming years. Research has shown that any degree of stress can have an impact on the pregnancy and child. This might range from minor stress (such as stress due to daily chores) to severe stress (such as bereavement, natural disasters/ terrorist attacks),
Adverse pregnancy and child development outcomes can result from stress during the entire pregnancy, including the third trimester.
How to relieve stress during pregnancy?
A) Identify the stressor:
Identifying and address the stressor should be the first step whenever possible. For example, speak with your Line Manager or Occupational Health Team. You might benefit from a temporary change of the type of work. Learning new time management skills could be helpful and allow you to have breaks at work.
B) Self-care:
Diet: A healthy nutritious diet is vital for physical and mental wellbeing. When going through a challenging phase, diet is often neglected. People might either not eat well or over-eat, including unhealthy food. Avoiding smoking, alcohol, and caffeine would be highly beneficial.
Exercise: Regular exercise helps in staying fit and improves wellbeing. Pregnancy yoga with good breathing techniques could be valuable.
Rest: Taking adequate rest during pregnancy is essential, especially when you are going through a stressful situation.
Pregnant women can suffer from sleep disturbance/ insomnia. Stress can aggravate the problem. Good sleep hygiene could be incredibly helpful.
Relaxation: To combat the stress and develop resilience, relaxation is vital. Whereas a good sleep (both quality and duration) can help our body to recover, good relaxation measures can help to cope better when we are awake.
– Meditation techniques, such as Mindfulness can be beneficial.
– Downloading some Apps could be helpful.
– ‘Me Time’: spending some time of the day doing things you enjoy, such as reading books, going for a walk or listening to a relaxing music.
– Taking a short-break or going on a holiday.
– Complementary therapies, such as EFT, massage, and reflexology, could be helpful.
C) Share your feelings:
Sharing your feelings with your partner, family members/ friends is valuable.
You can also meet other pregnant women in your Antenatal Classes. Some women join a local/ online pregnancy group.
Please take utmost care to ensure that this is a safe space to share your thoughts and confidentiality is maintained. For any online forum, please do relevant research, such as reading the Privacy Policy and reviews before you join and start participating on them.
D) Financial planning:
In some countries, women heavily rely on private healthcare providers for their antenatal care. This could be expensive.
Shopping for the newborn (such as buggies, cot, car seat, clothes, nappies or formula milk) could also cost a lot of money. Some women find it useful to look out for special offers. Some of the local/ national charities could help with basic accessories.
E) Psychological treatments:
– Guided Self-help techniques
– Counselling
– Cognitive Behavioural Therapy (CBT)
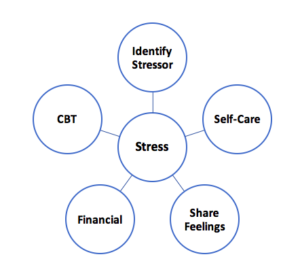
Reducing stress during pregnancy
Further reading on stress during pregnancy:
1. Book: Pregnancy Brain: A Mind-Body Approach to Stress Management During a High-Risk Pregnancy
2. Paper: Glover V. (2015) Prenatal Stress and Its Effects on the Fetus and the Child: Possible Underlying Biological Mechanisms. In: Antonelli M. (eds) Perinatal Programming of Neurodevelopment. Advances in Neurobiology, vol 10. Springer, New York, NY
3. Paper: Maternal depression, anxiety and stress during pregnancy and child outcome; what needs to be done. Glover, Vivette. Best Practice & Research Clinical Obstetrics & Gynaecology , Volume 28, Issue 1, 25 – 35
4. NHS Choices.
Reference
1. Kuo, C., Chen, G., Yang, M., Lo, H., Tsai, Y. (2000). Biphasic changes in the autonomic nervous activity during pregnancy. British Journal of Anaesthesia, 84, 323 – 329.
3. Taft A. Violence against women in pregnancy and after childbirth: current knowledge and issues in healthcare responses. Australian Domestic and Family Violence Clearinghouse Issues. Paper No. 6, University of New South Wales, Sydney 2002.
4. Department of Health. Improving Services for Women and Child Victims of Violence: Action Plan Department of Health, London 2010.

